Inflammation, Blood Vessels & the Eyelid Margin: What’s Really Causing Your Dry Eye?
- Michelle Carpenter

- 2 days ago
- 3 min read
Many people believe dry eye occurs simply because the eyes are not producing enough tears. In reality, one of the most common causes of chronic dry eye disease is inflammation along the eyelid margin.
Inflammation in this area disrupts the delicate balance of the tear film, damages the meibomian glands, and leads to progressive ocular surface irritation.
Understanding the relationship between eyelid margin inflammation, abnormal blood vessels, and gland dysfunction is key to identifying the root cause of chronic dry eye symptoms.
The Eyelid Margin: A Critical Area for Tear Film Health
The eyelid margin is the thin border where the eyelids meet the surface of the eye. This small anatomical area plays a major role in maintaining tear film stability.
Along the eyelid margin are the openings of the meibomian glands, which produce the oil layer of the tear film.
When these glands function normally, the oil layer slows evaporation and protects the ocular surface.
However, when inflammation develops along the eyelid margin, gland function becomes impaired.
Over time, this can lead to meibomian gland dysfunction (MGD) and evaporative dry eye.
Telangiectasia: The Abnormal Blood Vessels That Drive Inflammation
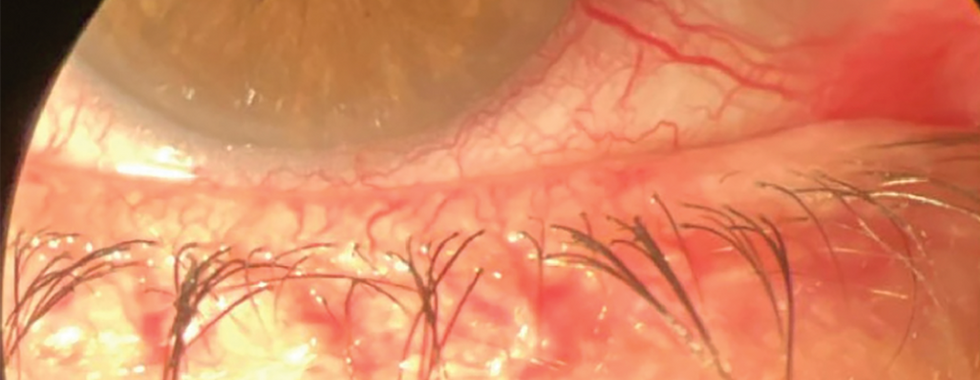
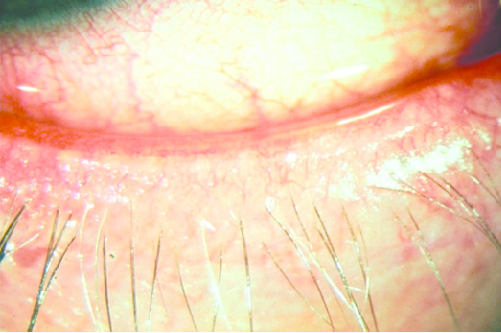
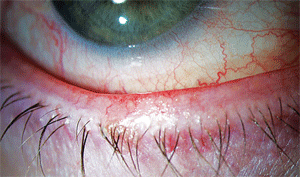
One of the most important clinical signs of inflammatory dry eye is the presence of telangiectasia, or abnormal dilated blood vessels along the eyelid margin.
These vessels are commonly associated with:
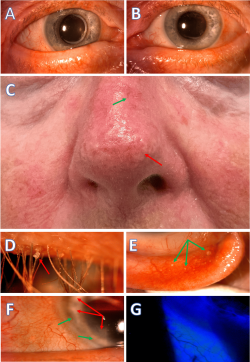
• Ocular rosacea• Chronic eyelid inflammation• Meibomian gland dysfunction• Long-standing evaporative dry eye
These vessels release inflammatory mediators that disrupt the glands responsible for producing the lipid layer of the tear film.
As inflammation increases:
• Oil quality deteriorates• Tear evaporation accelerates• The ocular surface becomes exposed• Symptoms intensify
How Eyelid Inflammation Leads to Dry Eye
Inflammation of the eyelid margin triggers a cascade of changes that ultimately destabilize the tear film.
These changes include:
• Thickening of meibomian gland secretions• Obstruction of gland openings• Reduced oil flow into the tear film• Increased tear evaporation• Ocular surface inflammation
This process explains why many patients experience dry eye symptoms even when tear production appears normal.
The issue is not simply tear quantity — it is tear film instability driven by inflammation.
Common Symptoms of Eyelid Margin Inflammation
Patients with inflammatory dry eye often report:
• Burning or stinging eyes• Red eyelid margins• Sensitivity to light• Fluctuating vision• Excessive tearing• Recurrent styes or chalazia• Irritation that worsens throughout the day
These symptoms frequently worsen with prolonged screen use, environmental exposure, or fatigue.
Diagnosing Inflammatory Dry Eye
Accurate diagnosis requires careful examination of both the ocular surface and eyelid structures.
Clinical evaluation may include:
• Eyelid margin examination• Meibomian gland expression• Tear break-up time measurement• Ocular surface staining• Assessment of inflammatory patterns
Identifying eyelid inflammation early helps prevent long-term gland damage.
Why Artificial Tears Often Fail
Artificial tears can temporarily supplement the aqueous layer of the tear film.
However, they do not address the inflammatory blood vessels along the eyelid margin that drive gland dysfunction.
Without treating the inflammatory source of disease, symptoms frequently return soon after drop use.
This is why patients often report only brief relief from lubricating drops.
Treating Eyelid Margin Inflammation
Effective treatment focuses on reducing inflammation and restoring gland function.
Modern therapies may include:
• Intense Pulsed Light (IPL) therapy• Thermal gland expression• Radiofrequency treatment• Anti-inflammatory management• Structured eyelid hygiene protocols
These treatments target both the inflammatory process and the gland obstruction that destabilize the tear film.
The Role of IPL in Treating Inflammatory Dry Eye
IPL therapy is one of the most effective treatments for inflammatory eyelid margin disease.
The treatment works by targeting abnormal blood vessels along the eyelid margin.
This helps:
• Reduce inflammatory mediator release• Improve meibomian gland oil quality• Restore tear film stability• Decrease ocular surface irritation
For patients with ocular rosacea and chronic eyelid inflammation, IPL can significantly improve both comfort and visual stability.
FLOW: Specialized Treatment for Inflammatory Dry Eye
Through FLOW, our dedicated ocular surface division serving Fort Worth and Dallas, we provide advanced evaluation and treatment for inflammatory dry eye disease.
FLOW integrates modern diagnostic technology with procedural therapies designed to restore gland health and stabilize the tear film.
By targeting inflammation at its source, this approach provides long-term improvement rather than temporary symptom relief.
Schedule a Dry Eye Evaluation in Fort Worth or Dallas
If you experience persistent burning, redness, or irritation, eyelid margin inflammation may be the underlying cause of your symptoms.
Our team provides comprehensive dry eye treatment in Fort Worth and Dallas, evaluating gland health, tear film stability, and inflammatory patterns to determine the most effective treatment plan.
Schedule an evaluation to restore ocular surface health and achieve lasting relief from chronic dry eye.








Comments